 Your new post is loading...
 Your new post is loading...
Treatment with a next-generation CAR T-cell agent displayed early efficacy in a small group of patients with glioblastoma.
Targeting two brain tumor-associated proteins-;rather than one-;with CAR T cell therapy shows promise as a strategy for reducing solid tumor growth in patients with recurrent glioblastoma (GBM), an aggressive form of brain cancer, according to early results from the first six patients treated in an ongoing Phase I clinical trial led by researchers from the Perelman School of Medicine at the University of Pennsylvania and Penn Medicine's Abramson Cancer Center.
Siteman Cancer Center, based at Barnes-Jewish Hospital and Washington University School of Medicine in St. Louis, is one of the first centers nationwide to offer a newly approved cell-based immunotherapy that targets melanoma.
Immunotherapy using modified chimeric antigen receptor (CAR) T cells has greatly improved survival rates for pediatric patients with relapsed and recurrent leukemia.
In the context of relapsed and refractory childhood pre-B cell acute lymphoblastic leukemia (R/R B-ALL), CD19-targeting chimeric antigen receptor (CAR)-T cells often induce durable remissions, which requires the persistence of CAR-T cells. In this study, we systematically analyzed CD19 CAR-T cells of 10 children with R/R B-ALL enrolled in the CARPALL trial via high-throughput single-cell gene expression and T cell receptor sequencing of infusion products and serial blood and bone marrow samples up to 5 years after infusion. We show that long-lived CAR-T cells developed a CD4/CD8 double-negative phenotype with an exhausted-like memory state and distinct transcriptional signature. This persistence signature was dominant among circulating CAR-T cells in all children with a long-lived treatment response for which sequencing data were sufficient (4/4, 100%). The signature was also present across T cell subsets and clonotypes, indicating that persisting CAR-T cells converge transcriptionally. This persistence signature was also detected in two adult patients with chronic lymphocytic leukemia with decade-long remissions who received a different CD19 CAR-T cell product. Examination of single T cell transcriptomes from a wide range of healthy and diseased tissues across children and adults indicated that the persistence signature may be specific to long-lived CAR-T cells. These findings raise the possibility that a universal transcriptional signature of clinically effective, persistent CD19 CAR-T cells exists. In children with relapsed or refractory B cell acute lymphoblastic leukemia and in complete remission after CD19 CAR-T cell therapy, long-lived CAR-T cells express a persistence gene signature that is also present in persistent CD19 CAR-T cells from adults with chronic lymphocytic leukemia.
Three young patients with relapsed T-cell leukemia have now been treated with base-edited T-cells, as part of a 'bench-to-bedside' collaboration between UCL and Great Ormond Street Hospital for Children (GOSH).
Adoptive transfer of genetically engineered chimeric antigen receptor (CAR) T cells is becoming a promising treatment option for hematological malignancies. However, T cell immunotherapies have mostly failed in individuals with solid tumors. Here, with a CRISPR–Cas9 pooled library, we performed an in vivo targeted loss-of-function screen and identified ST3 β-galactoside α-2,3-sialyltransferase 1 (ST3GAL1) as a negative regulator of the cancer-specific migration of CAR T cells. Analysis of glycosylated proteins revealed that CD18 is a major effector of ST3GAL1 in activated CD8+ T cells. ST3GAL1-mediated glycosylation induces the spontaneous nonspecific tissue sequestration of T cells by altering lymphocyte function-associated antigen-1 (LFA-1) endocytic recycling. Engineered CAR T cells with enhanced expression of βII-spectrin, a central LFA-1-associated cytoskeleton molecule, reversed ST3GAL1-mediated nonspecific T cell migration and reduced tumor growth in mice by improving tumor-specific homing of CAR T cells. These findings identify the ST3GAL1–βII-spectrin axis as a major cell-intrinsic program for cancer-targeting CAR T cell migration and as a promising strategy for effective T cell immunotherapy. CAR T cell success requires targeting tumors, but these cells can get trapped in other tissues, such as in the lungs, where they can cause pathology. Here, the authors use a loss-of-function CRISPR screen to identify regulators of CAR T cell tumor trafficking and engineer CAR T cells accordingly to overcome this limitation.
Adding a molecular anchor to the key protein used to recognize cancer in cellular immunotherapies can make the treatments significantly more effective.
The recent years have seen a wave of adoptive cell therapies (ACTs), a type of immunotherapy in which T cells (T cell transfer therapy) and other immune cells are obtained from patients, activated and multiplied outside the body, and infused in larger numbers back into the blood circulation to help fight cancers.
Last week, PACT Pharma shared results from the first clinical trial using CRISPR to direct patients’ immune cells to treat solid tumours. The findings, which were published in an unedited manuscript in Nature, provide early proof-of-concept that patient immune cells can be reprogrammed to attack their own cancer. The results were als
A new approach to cancer immunotherapy that uses one type of immune cell to kill another-;rather than directly attacking the cancer-;provokes a robust anti-tumor immune response that shrinks ovarian, lung, and pancreatic tumors in preclinical disease models, according to researchers at the Icahn School of Medicine at Mount Sinai in New York.
Scientists at St. Jude Children's Research Hospital identified a molecular mechanism that in a preclinical study unlocked the promise of CAR T–cell therapy for treatment of solid tumors.
|
Magnetic resonance imaging (MRI) and lumbar puncture (LP) may not always be necessary for diagnosing and managing a serious neurological complication associated with CAR T-cell therapy, according to a new Blood Advances study.
Over the past two decades, the immune system has attracted increasing attention for its role in fighting cancer.
Chimeric antigen receptor T-cell therapy, or CAR T, has dramatically improved the treatment of certain blood cancers. Initially approved for patients who had failed multiple lines of therapy, clinical trials have shown CAR T can be used as an earlier treatment option.
At EPFL's School of Engineering, Professor Li Tang's Laboratory of Biomaterials for Immunoengineering has made significant strides in cancer treatment research.
A broad new strategy could hold hope for treating virtually all blood cancers with CAR T cell therapy, which is currently approved for five subtypes of blood cancer.
Vaccine boosting modifies CAR T cell metabolism and promotes crosstalk between CAR
T cells and endogenous immunity to elicit and sustain antigen spreading, thereby effectively
treating tumors with antigen heterogeneity.
Chimeric antigen receptors (CARs) and synthetic Notch (synNotch) receptors are engineered cell-surface receptors that sense a target antigen and respond by activating T cell receptor signaling or a customized gene program, respectively. Here, to expand the targeting capabilities of these receptors, we develop “universal” receptor systems for which receptor specificity can be directed post-translationally via covalent attachment of a co-administered antibody bearing a benzylguanine (BG) motif. A SNAPtag self-labeling enzyme is genetically fused to the receptor and reacts with BG-conjugated antibodies for covalent assembly, programming antigen recognition. We demonstrate that activation of SNAP-CAR and SNAP-synNotch receptors can be successfully targeted by clinically relevant BG-conjugated antibodies, including anti-tumor activity of SNAP-CAR T cells in vivo in a human tumor xenograft mouse model. Finally, we develop a mathematical model to better define the parameters affecting universal receptor signaling. SNAP receptors provide a powerful strategy to post-translationally reprogram the targeting specificity of engineered cells. Chimeric antigen receptors (CARs) and synthetic Notch (synNotch) receptors are promising platforms for cell-based immunotherapies. Here, the authors develop highly programmable versions of these receptors that can be universally targeted to antigens of interest through covalent enzyme chemistry.
A new approach that delivers a "one-two punch" to help T cells attack solid tumors is the focus of a preclinical study by researchers from the Perelman School of Medicine at the University of Pennsylvania.
With a slew of tools to trick out immune cells, researchers are expanding the repertoire of CAR-T therapies.
In two separate studies, researchers demonstrate how synthetic biology can be used to tackle a difficult issue in cancer immunotherapy: the way immunotherapy-related approaches focused on short-term killing of tumor cells may fail to eradicate tumors because growth of tumors happens on longer timescales.
Researchers at Great Ormond Street Hospital for Children (GOSH) and UCL Great Ormond Street Institute of Child Health (UCL GOS ICH) have used CRISPR/Cas9 technology to engineer donor T cells to try to treat seriously ill children with resistant leukaemia, who had otherwise exhausted all available therapies.
‘Most complicated therapy ever’ tailors bespoke, genome-edited immune cells to attack tumours.
|



 Your new post is loading...
Your new post is loading...

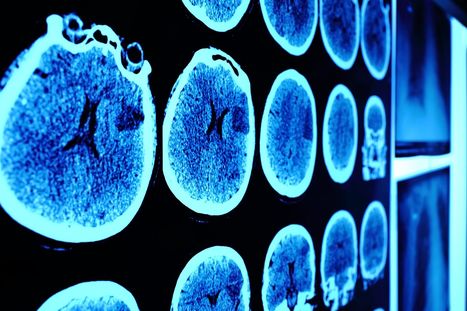














CARv3-TEAM-E T cells are CAR T cells targeting EGFR variant III tumor-specific antigen (EGFRvIII) in addition to wild-type EGFR. According to the results of the phase 1 INCIPIENT trial (NCT05660369) published in the New England Journal of Medicine, preliminary results in humans demonstrated that all 3 glioblastoma patients treated with CARv3-TEAM-E T cells between March 2023 and July 2023 showed dramatic and rapid radiographic regression of their tumors within days of receiving CARv3-TEAM-E T cells via a single intraventricular infusion. Responses were transient in 2 of the patients, however 1 patient, a 72-year-old man, showed an 18.5% decrease in tumor cross-sectional area on day 2 after receiving a single infusion of 10 x 106 CAR-positive CARv3-TEAM-E T cells. Moreover, 69 days after infusion, tumor cross-sectional area had decreased by a further 60.7% from baseline; the response was sustained and continued to improve at the last assessment, which took place more than 150 days after infusion.